The first sting of the drink is always the most vivid. A thin rim of cold glass against your lip, the quiet clink of ice, that soft rush of warmth as it unspools down your throat. Maybe it’s a beer after mowing the lawn, a glass of red with dinner, a gin and tonic catching the light of a late summer evening. It all feels so ordinary, almost harmless—woven into the background hum of daily life. You raise the glass, swallow, and move on. But somewhere, in that brief contact between liquid and flesh, a quieter story might be unfolding, one that begins in the tissue of your mouth and could end, years later, in a doctor’s office with a word you never imagined would belong to you: cancer.
The Quiet Places Alcohol Touches
We tend to think of alcohol as something that happens in the stomach, the liver, the brain. A fuzzy head, a queasy gut, a hangover. But the first place alcohol lands is the soft, vulnerable lining of your mouth—your tongue, your cheeks, your gums, your throat. These surfaces are as alive and busy as a forest floor, cells dividing and renewing, repairing tiny injuries you never notice, quietly tending to the work of being your first line of defense against the world.
When alcohol hits this delicate landscape, it doesn’t simply pass by like a polite guest. Ethanol—the kind of alcohol in your drink—is a small, reactive molecule. Enzymes in your mouth and upper airways begin breaking it down almost immediately, and in that process a new compound is born: acetaldehyde. The name sounds technical, forgettable, but the body remembers it with a kind of alarm. Acetaldehyde is toxic. It can damage DNA, the coded instructions that tell your cells when to grow, when to rest, when to die.
Most of the time, your body is good at cleaning up these messes. Repair systems flicker on, damaged cells are ushered quietly out of circulation, new cells step in. But those systems work best under light use, like a trail occasionally traveled. When alcohol appears every day—just one drink, the “moderate” kind we’re told is safe—the trail turns into a road, then a well-worn highway. The exposure is no longer fleeting; it’s habitual. And that’s when the risk begins to shift.
When “Moderate” Isn’t So Mild
You’ve probably heard the old comfort phrases: “Everything in moderation.” “A glass a day is fine.” For years, moderate drinking was painted as almost virtuous, even protective, especially when attached to a glass of red wine and a Mediterranean sunset. The cultural story was appealing: you can drink a little, even daily, and perhaps even live longer.
But nature doesn’t follow our stories—it follows chemistry and time. Over the past decade, research has grown more precise, and the picture it paints is stark: when it comes to certain cancers, including mouth and throat cancers, there may not be a truly safe level of alcohol use. Even light drinking—about one drink a day—has been associated with an increased risk.
Imagine you’re watching a forest over many seasons. A single spark in the undergrowth might die out quickly, smothered by damp soil and green leaves. But if that spark returns day after day in the same patch of brush, some days bigger, some days smaller, the plants there become dry, thin, more vulnerable. Eventually, it doesn’t take a raging wildfire to ignite disaster; a slow ember is enough.
Your mouth is that forest, and daily alcohol is the recurring spark. One drink a day won’t guarantee a fire—not even close. Most people who drink lightly will never develop mouth cancer. But the quiet math of risk is still shifting under the surface, and that shift is worth listening to.
The Body’s Uneasy Truce with Alcohol
Inside your cells, acetaldehyde behaves like a vandal. It can bind to DNA and the proteins that help your DNA fold and function, forming awkward links that confuse the normal order of things. When your cells try to divide, they must copy this compromised DNA, and errors begin to slip through. One error isn’t usually enough to tip a cell into cancer, but each damage event is like adding a stone to a precarious pile. Over years and decades, the stack can become unstable.
Enzymes like ALDH2 usually race to clean up acetaldehyde, converting it into safer compounds. But not all bodies are equally equipped. Some people, particularly many of East Asian descent, have genetic variants that make this cleanup crew sluggish. They may experience facial flushing, a racing heartbeat, or nausea when they drink—all warning signs that acetaldehyde is hanging around too long. Yet even for those who don’t feel it, the invisible chemistry is still at work.
The lining of the mouth is often exposed to other insults too: tobacco smoke, spicy foods, sharp edges of teeth, chronic irritation from ill-fitting dentures. Alcohol can act like a solvent, helping other harmful substances penetrate deeper into tissues. For those who smoke and drink, the risk isn’t just added—it can multiply. In that layered environment, even “just one” becomes part of a larger, riskier ecosystem.
The Numbers Beneath the Glass
Risk, when translated into human lives, can feel abstract. So researchers try to capture it in numbers: relative risk, absolute risk, percentages, rates. These can sound cold, but if you lean in, they tell a quiet story about how many people in a room, a town, a lifetime might be affected.
For mouth and throat cancers, studies have found that even light drinkers—often defined as up to one drink per day—have a higher risk than people who don’t drink at all. The increase may not sound dramatic on paper, but remember: cancer is already a rare event. Any shift upward, especially over a lifetime, matters.
To help make these patterns more tangible, here is a simplified way of looking at how drinking level relates to mouth and throat cancer risk. These are not exact predictions for any one person, but they outline how the risk landscape tends to tilt.
| Drinking Pattern | Typical Amount | Relative Risk vs. Non-Drinkers* | How to Picture It |
|---|---|---|---|
| No alcohol | 0 drinks | Baseline (1.0) | Your starting line; risk is not zero, but lower. |
| Light drinking | About 1 drink/day | Slightly above 1.0 | A modest but real upward nudge in risk. |
| Moderate drinking | 2–3 drinks/day | Noticeably higher | Imagine several more people in a crowd developing cancer. |
| Heavy drinking | 4+ drinks/day | Substantially higher | Risk can be several times that of non-drinkers. |
*Relative risk here is simplified for illustration; exact figures vary by study, genetics, tobacco use, and other factors.
If you imagine a hundred people who never drink, some small number of them may still develop mouth or throat cancer in their lifetime. Now imagine another hundred who each drink a single drink every day. In that second group, more people will develop these cancers. Not dozens more, not half the room—but enough to matter, especially when you zoom out to entire populations, cities, countries.
Listening to the Early Whispers
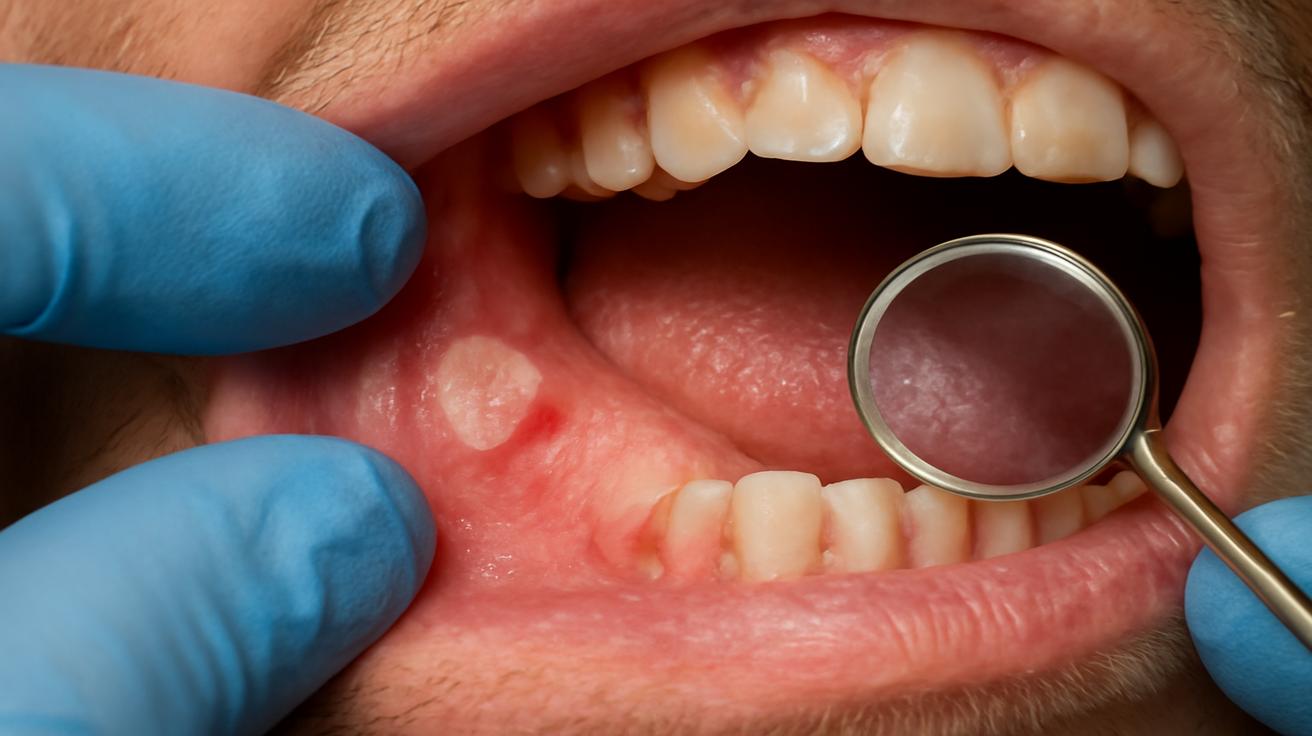
Cancer, especially in the mouth, rarely appears overnight. The body tends to whisper before it shouts. White or red patches on the tongue or the inside of the cheek. A sore that lingers week after week instead of healing. A little difficulty swallowing that you explain away as “I must have eaten too fast.” A numb spot, a thickening, a subtle change in how your teeth fit together.
For those who drink daily, even lightly, these whispers carry extra weight. The risk is higher, which doesn’t mean doom—it means attention becomes an act of self-respect. Dentists often see the earliest signs of trouble; they peer at your tongue and gums under bright light, noticing subtle shifts you might miss. Regular checkups, the kind that feel routine or tedious, can quietly become life-saving.
Yet early detection is only one part of the story. The other part is prevention—asking what we’re willing to shift in our daily rituals long before we’re sitting in a waiting room under fluorescent lights, cataloging all the ways we thought “just one” would never matter.
Redrawing Your Evening Ritual
Picture your usual drinking moment. Maybe it’s the soundscape first: a pan sizzling, a television murmuring, crickets outside a kitchen window. The small ceremony of twisting a bottle cap, uncorking a wine bottle, or measuring a clear spirit into a glass. It’s not only the alcohol you reach for. It’s the signal that the workday is over, that you’re allowed to exhale, that you’re stepping into a softer chapter of the day.
What happens if that ritual changes shape?
For some, cutting back might begin with curiosity, not punishment. What does an evening feel like with a sparkling water in a heavy glass, a squeeze of lime, and a sprig of mint you bruised gently between your fingers? Can the same sense of ceremony exist if the drink isn’t quietly etching its name into your cells? You might notice different things when you’re not under alcohol’s soft blur: the way the light slants through the window, the subtleties of taste in your food, the cadence of a conversation that doesn’t drift into fog.
On a deeper level, stepping back from daily drinking is often less about alcohol and more about what you’ve asked it to carry. Stress relief. Social ease. A shield against boredom or loneliness. When you begin to adjust your relationship with that one drink, you’re often adjusting your relationship with the parts of life that feel sharp or empty. That’s hard, and also quietly radical.
The Small Choices That Bend the Curve
If your daily drink has been part of your life for years, imagining a different pattern might feel like trying to reroute a river with your bare hands. But rivers are shaped not by a single stone, but by many small shifts over time.
Some people find it more realistic to start with these kinds of changes:
- Choosing at least a few alcohol-free days each week, and treating them as normal, not as deprivation.
- Switching to smaller pours—less wine in the glass, a single beer instead of a tall one, more mixer and less spirit.
- Keeping non-alcoholic options visible and ready: herbal teas, flavored sparkling waters, or well-crafted alcohol-free drinks.
- Not drinking automatically with every dinner, but choosing it more deliberately on certain occasions.
Each small shift nudges your lifetime exposure a little lower. The body is remarkably forgiving when given the chance. Quit or cut back early enough, and in many cases your risk can begin to move closer to that of someone who never drank at all, especially if you don’t smoke and you care for your oral health.
A More Honest Kind of Comfort
It’s tempting to seek reassurance that a single daily drink is harmless—that there’s a neat line between “safe” and “unsafe,” and that you’re comfortably on the safe side. But the natural world, including the world inside your own mouth, doesn’t tend to draw such crisp borders. Risk behaves more like a gradient, a slow shift in shade from light to dark.
A more honest comfort might sound like this: there is no guaranteed safe amount of alcohol when it comes to cancers of the mouth and throat, but your choices still matter deeply. Every drink you don’t have reduces your lifetime exposure. Every year you live with less alcohol on your tongue, every evening you spend with a different kind of glass in your hand, tilts the odds a little more in your favor.
There’s also comfort in remembering that you’re not fragile glass, doomed to shatter with one wrong move. You are a living system, adaptable, resilient, capable of change. Your mouth has its own seasons of damage and repair, of injury and healing. The question is less “Have I already ruined something?” and more “What kind of environment do I want to offer my cells from this point forward?”
In the end, the story of that “one drink a day” isn’t a morality tale about virtue and vice. It’s a story about attention—about noticing what we’ve normalized, and deciding, gently, whether the quiet cost is one we’re still willing to pay. When you lift a glass to your lips, you’re not just tasting this moment; you’re also, in a small way, writing your body’s future chapters.
Some future evening, you might sit at the same table, the same light catching the curve of a glass. Maybe the glass will hold wine. Maybe it will hold something else—something that doesn’t leave a chemical echo on your cells. Either way, you’ll know more than you did before. You’ll know that even a single daily drink can bend the risk lines in your body, tracing a faint path toward cancers no one ever plans for. And with that knowledge, you’ll also hold a quieter power: the power to choose, with eyes open, what story you want your next sip to tell.
Frequently Asked Questions
Does one drink a day really increase my risk of mouth cancer?
Yes. Research suggests that even light drinking—around one standard drink per day—is associated with a higher risk of cancers of the mouth and throat compared with not drinking at all. The increase is modest for an individual, but it’s real and becomes more significant over many years.
What counts as “one standard drink”?
Roughly speaking, one standard drink is about:
- 350 ml of regular beer
- 150 ml of wine
- 45 ml of distilled spirits (like vodka, gin, or whiskey)
Glasses and pours at home are often larger than this, so many people drink more than they realize.
If I only drink on weekends, is that safer than a drink every day?
Spreading alcohol across fewer days but in larger amounts can bring other risks, like accidents and acute health problems. From a cancer perspective, the total amount you drink over time matters. Drinking less overall—fewer drinks in total per week or month—is generally better for lowering cancer risk.
Can stopping or cutting back reduce my risk, even if I’ve been drinking for years?
Yes. While past exposure can’t be erased, cutting back or quitting can lower your future risk. Over time, especially if you also avoid tobacco and maintain good oral health, your risk of mouth and throat cancer can move closer to that of someone who drinks little or not at all.
What early signs of mouth cancer should I watch for?
Watch for:
- Persistent sores or ulcers in the mouth that don’t heal within two weeks
- White or red patches on the tongue, gums, or inside the cheeks
- Unexplained pain, numbness, or a lump in the mouth or neck
- Difficulty chewing or swallowing
- Changes in your voice or a persistent sore throat
If you notice any of these for more than a couple of weeks, see a dentist or doctor promptly.
Does the type of alcohol matter—beer, wine, or spirits?
For mouth and throat cancers, the main issue is the ethanol itself, not the type of drink. Beer, wine, and spirits all contain alcohol, and all can raise risk. Some patterns of drinking may differ by beverage type, but no form of alcohol is truly “safe” for oral cancer risk.
I don’t want to quit completely. Is there still a benefit to just cutting down?
Absolutely. Any reduction in the amount and frequency of alcohol you drink reduces your cumulative exposure and can help lower your risk. Fewer drinks per week, more alcohol-free days, and smaller pours are all meaningful steps in a healthier direction.